CHAPTER 4
RECOMMENDATIONS ON NUTRITION

The remarks of the present chapter are based to a large extent on a report of a special World Health Organization study group on “Diet, Nutrition and the Prevention of Chronic Diseases” published in 1990 and a follow up report of a joint WHO/FAO 1) Food and Agriculture Organization of the United Nations. expert consultation twelve years later. At the inaugural session Dr. Hu Ching-Li, representative of the WHO, said: “The amount and type of food eaten are fundamental determinants of human health.”
A few pages ahead we read that “a range of chronic diseases can be prevented to a substantial extent by life-style changes, among which diet plays a crucial role.” (Diet, Nutrition, and the Prevention of Chronic Diseases, WHO, 1990, p. 39)
Diet and Chronic Diseases
The main causes of death in developed countries are cardiovascular diseases and cancer. Both together make up grossly three quarts (75%) of all deaths. There is not much difference between West and East Europe as can be seen in the following graphics; and since the risk factors of these diseases are basically the same, we can study them together.
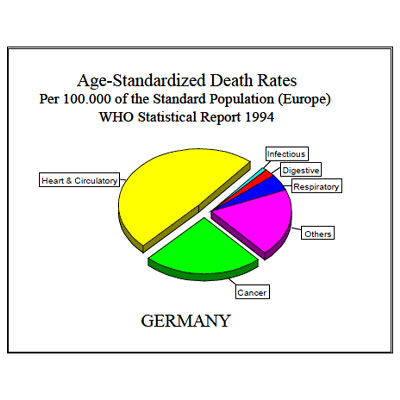
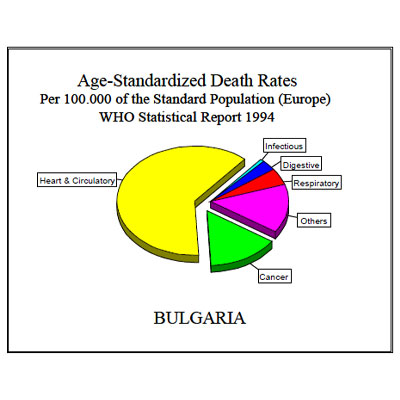
In first place it was noticed that there were “inappropriate public perceptions in developing countries of what constitutes a better diet, … with high contents of fat, sugar, and salt.” (Diet, Nutrition, and the Prevention of Chronic Diseases, WHO, 1990, p. 15) At the same time the risk factors for cardiovascular diseases and cancer are precisely related to such diet:
- excess of fat
- excess of free sugars
- deficiency of complex carbohydrate foods
- cigarette smoking
Diet, Nutrition, and the Prevention of Chronic Diseases, WHO, 1990, p. 11, 56)
They also realized that “these chronic diseases [coronary heart disease, cancer, hypertension, diabetes] are, in part, manifestations of nutrient excesses and imbalances in the »affluent« diet, so they are in principle, largely preventable.” (Id, p. 14)
By way of contrast, “a substantial amount of epidemiological and clinical data indicates that a high intake of plant foods and complex carbohydrates is associated with a reduced risk of several chronic diseases, especially coronary heart disease, certain cancers, hypertension, and diabetes.” (Id, p. 99)
Consequently, “in several Western European countries and in North America, there have been sustained public education campaigns, that aim to change the public’s eating patterns. … Unfortunately, the idea that medical opinion is divided and that policies are uncertain is often used to inhibit change, despite the remarkable consistency of views put forward by expert groups over several decades.” (Id, p. 129)
It is sad to realize that many wives and mothers are not aware that the health of their spouse and children depends largely upon the food they prepare for their families. Here are some pertinent counsels:
“There are very many girls who have married and have families, who have but little practical knowledge of the duties devolving upon a wife and mother. They can read, and play upon an instrument of music; but they cannot cook. They cannot make good bread, which is very essential to the health of the family. … To cook well, to present healthful food upon the table in an inviting manner, requires intelligence and experience. The one who prepares the food that is to be placed in our stomachs, to be converted into blood to nourish the system, occupies a most important and elevated position. The position of copyist, dress-maker, or music teacher cannot equal in importance that of the cook.” (Testimony Studies on Diet and Foods, p. 94)
“It is sacred duty for those who cook to learn how to prepare healthful food. Many souls are lost as the result of poor cookery. It takes thought and care to make good bread; but there is more religion in a loaf of good bread than many think. There are few really good cooks. Young women think that it is menial to cook and do other kinds of housework; and for this reason, many girls who marry and have the care of families have little idea of the duties devolving upon a wife and mother. Cooking is no mean science, and it is one of the most essential in practical life. Every woman who is at the head of a family and yet does not understand the art of healthful cookery should determine to learn that which is so essential to the well-being of her household.” (Ministry of Healing, p. 302)
The present chapter does not pretend to be a detailed textbook on nutrition but rather I would like to emphasize some major aspects that are commonly misunderstood.
Cancer and Diet
Is there any relation between cancer and diet? Can the risk of cancer be reduced by diet? To begin, here are some statements from scientific authorities.
“Vegetables and fruits are a rich source of a number of nutrients. […] There is consistency in the evidence that vegetables and fruits play some protective role in preventing the development of cancers.” (Diet, Nutrition, and the Prevention of Chronic Diseases, WHO, 1990, p. 98)
The director of the National Cancer Institute’s division of Cancer Prevention and Control of the USA concluded: “A greater number of studies have shown that a diet rich in fruits and vegetables has a protective effect against cancer. Persons with high fruit and vegetable intakes have about half the risk of people with low intakes.” (Better Nutrition, May 1994, p. 20)
Finally here is an important inspired statement from Ellen G. White that is fully in accordance with the previous assertions: “Cancer, tumors, and all inflammatory diseases are largely caused by meat-eating. From the light which God has given me, the prevalence of cancers, and tumors is due to gross living on dead flesh.” (Spalding and Magan Collection, p. 47)
It is interesting to notice that E. G. White also mentions “inflammatory” diseases. “The Adventist Health Study reported a 50% greater prevalence of rheumatoid arthritis and other forms of arthritis among non-vegetarians compared with vegetarians. … The mechanisms have not been explained yet.” (Gary E. Fraser, Diet, Life Expectancy and Chronic Disease, 2003, p. 144-146)
Fats and Cholesterol
For the understanding of this section we presuppose a basic knowledge about fats. We will limit our explanations to some facts related to chronic diseases.
It is well documented that high serum cholesterol levels are a risk factor for coronary heart disease. The usually considered “normal” values of 200 mg% are too high. Ideally the serum cholesterol level should be 150 mg% or lower. This may sound frightening because very few people in Western societies have such low values.
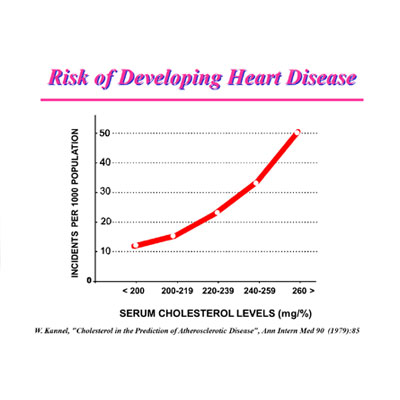
When studies showed that a high consumption of saturated fats, mostly of animal origin, tends to raise serum cholesterol levels, a movement begun towards the use of polyunsaturated fats, as found in corn oil, sunflower oil and others, because they tend to lower blood cholesterol levels. Care must be taken, however, because polyunsaturated oils, including omega-3 fatty acids, are not very stable. Soon margarine appeared on the market to substitute butter. However, the issue relating to fats is not that simple. Persons with high cholesterol levels should avoid all animal fats (butter, meat, cheese) in first place, because cholesterol is found ONLY in animal products. Besides of that, the total amount of fat consumed should be reduced. In a typical Western cuisine the total consumption of fat is too high.
Heating and frying fats, especially polyunsaturated oils, should be minimized because heating may produce trans-fatty acids and other harmful substances. This is one reason why cold pressed extra virgin oils are better than oils extracted using heat. It is a bad sign when oils begin to smoke when heated. Coconut oil and peanut oil are the most stable; then comes olive oil. Sunflower, canola and corn oils are therefore not appropriate for heating. Onions and peppers can also be sautéed in water instead of oil.
Trans-fatty acids do not occur in nature, they are the result of artificial processing. “Fast foods, chips, baked goods, and other commercially prepared foods are high in fats containing up to 50 percent trans-fatty acids. Overall, consumers are eating more fats containing trans-fatty acids than ever before and they are eating them in the form of processed foods.” (Sizer & Whitney, Nutrition – Concepts and Controversies, p. 166)
Trans-fatty acids tend to raise LDL-cholesterol and lower HDL-cholesterol. Instead of acting as the natural cis fatty acids, trans fatty acids compete and hinder them. There is a consensus that trans-fatty acids increase the risk of both, cardiovascular diseases and cancer. Today, the labels must show the amount of trans-fatty acids contained in industrial foods.
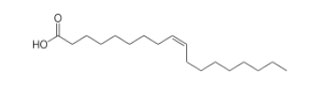
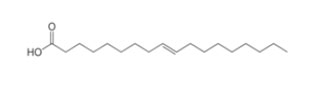
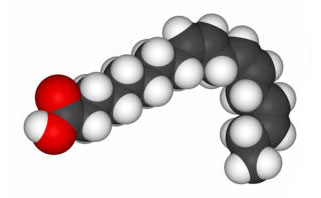
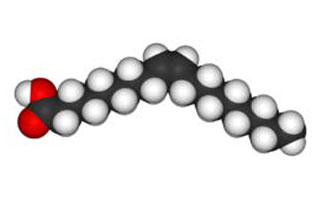
Unsaturated Fatty Acids
| Cis | Cis | Trans |
|---|---|---|
 |
 |
 |
 |
 |
 |
|
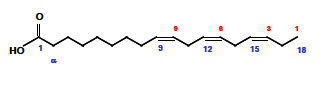
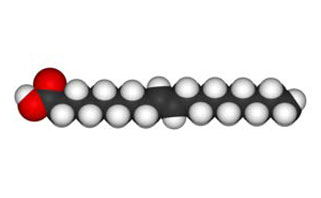
Alpha-linolenic acid is a polyunsaturated omega-3 cis-fatty acid. It is found in many common vegetable oils and is important to human nutrition. |
Oleic acid is a cis-fatty acid, contained by 55-80% in olive oil. The melting point is at 13.5 °C. |
Elaidin acid is a trans-fatty acid contained in milk and is also found in hydrogenated plant oils. The melting point is at 46.5 °C. |
(Wikipedia)
At this point we must mention the omega-3 and omega-6 fatty acids. These essential fatty acids are not new. They are present in linseed, nuts, soybeans, seeds, and other vegetable foods. There is now more knowledge about the mechanisms of their actions in health and disease. Fish get the α-linolenic acid (ALA) from algae and transform it in their body into eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA) that are physiologically more active. Researchers believe the ideal omega-6 intake should be no more than 4-5 times that of our omega-3 intake. The media and industry took chance of these “new discoveries” and now encourage eating more fish or taking supplements of fish oil. However, “consumers of oily fish should be aware of the potential presence of heavy metals, in particular mercury, lead, nickel, arsenic and cadmium, and fat-soluble pollutants like PCBs [polychlorinated biphenyls] and dioxins which may accumulate up the food chain.” (www.fda.gov/bbs/topics/news/2004/NEW01115.html, US Food and Drug Administration)
“Omega supplementation in food has been a significant recent trend in food fortification, with global food companies launching omega-3 fortified bread, pizza, yoghurt, orange juice, children’s pasta, milk, confections and infant formula.” (Wikipedia)
It is not necessary to resort to fish or fish oil supplements in order to get sufficient amount of essential fatty acids in the right proportion. Flax (Linum usitatissimum) and its oil are perhaps the most widely available botanical source of omega-3. Flaxseed oil consists of ca. 55% ALA (α-linolenic acid) in a proportion of 3 times as much omega-3 as omega-6. However, we must be aware that flax seed oil becomes rancid very fast and should always be freshly prepared and used within three weeks. The easiest and more practical way perhaps is to mill the flax seeds (1 tablespoon) in a small coffee mill just before eating and spread this powder over the breakfast cereal or foods at lunch. There is plenty of omega-3 in walnuts, soybeans and dark leafy vegetables.
To conclude this section it is worth to pay attention to the following wise counsels of Ellen G. White:
“When properly prepared, olives, like nuts, supply the place of butter and flesh meats. The oil, as eaten in the olive, is far preferable to animal oil or fat. It serves as a laxative. Its use will be found beneficial to consumptives, and it is healing to an inflamed, irritated stomach.” (Ministry of Healing, p. 298)
“Food should be prepared with simplicity, yet with a nicety which will invite the appetite. You should keep grease out of your food. It defiles any preparation of food you may make. Eat largely of fruits and vegetables.” (Counsels on Diet and Foods, p. 200)
“Your appetites are morbid, and because you do not relish a plain, simple diet, composed of unbolted wheat flour, vegetables and fruits prepared without spices or grease, you are continually transgressing the laws which God has established in your system. While you do this, you must suffer the penalty; for to every transgression is affixed a penalty. Yet you wonder at your continued poor health.” (Counsels on Diet and Foods, p. 123)
Calcium and Osteoporosis
Almost every mature adult and elderly person in the western world today is concerned about osteoporosis. What is the reason? Popular health magazines have headlines on the prevention of osteoporosis; advertising of calcium supplements and dairy products are increasing, but osteoporosis is still becoming more frequent. This issue is on hot debate. However, there are some unequivocal facts that should be considered.
First of all, what are the factors contributing to osteoporosis? The WHO study group mentions several main factors involved in calcium metabolism:
- lack of estrogen
- immobility
- smoking
- alcohol
- calcium intake
And they explain that “it is by no means certain that calcium intake is the key feature determining bone density and bone loss in adult life. High-protein and high-salt diets are known to increase bone loss.” (Diet, Nutrition, and the Prevention of Chronic Diseases, WHO, 1990, p. 82)
Lack of exercise is one of the important risk factors and is being stressed more and more. But have you ever heard that smoking and alcohol promote osteoporosis? This fact is taboo. What about high-protein diets?
Linkswiler did an experiment on calcium balance comparing 3 groups of people. They all consumed 1400mg of calcium per day. But their protein intake was different. The group that received only 48 g of protein/day showed a positive calcium balance whereas the groups receiving more protein showed calcium loss proportional to their protein intake. (Linkswiler HM, Protein-induced hypercalciuria, Fed Proc 1981 Jul; 40 (9): 2429-2433)
A high protein intake also increases the risk of kidney stones.
The recommended daily allowance (RDA) for calcium vary greatly according to different countries. For example, the USA and Germany recommend 1200 mg for adults, including pregnant or lactating women. Such high amount cannot be reached by vegetarians without including dairy products into their diet or without taking calcium supplements. The WHO recommends only 400-500 mg daily.

It is also known that high phosphorus intake promotes calcium loss. The major sources of phosphorus are meat and dairy products.
Another study was done by Marsch und Sanchez who examined the mineral content of the bones of 1600 women. At age 60 these women still had the full mineral content. Twenty years later they were examined again. The ladies using a lacto-ovo-vegetarian diet still had 82% of their mineral content whereas those with a mixed diet, containing also meat, had only 65% left. (A. Marsh, T. Sanchez, Vegetarian lifestyle and bone mineral density, American Journal of Clin. Nutr. 1988; 48)

The Calcium Paradox
Let’s talk about some important concepts in medicine. You may have noticed in the beginning of this chapter the words “imbalances” and “excesses”. In the past, science was concerned with diseases caused by nutritional “deficiencies”. Consequently the minimum daily needs were determined and people were happy to get as much as possible; the more the better. This idea was found to be wrong. For good health everything must stay within a certain normal range; not more and not less. But what is normal and how can it be determined? Usually, a group of apparently healthy people are taken and their average values were considered as normal. Later it was found that other groups of also healthy people, sometimes in other areas of the world, had quite different values. Just as an example, can we say that serum cholesterol levels of 200 mg% are normal for Americans and abnormal for Japanese? Are human beings that different? This shows that we are continuously learning and what was considered normal in the past may not be considered as normal today.
Another important point is that nutrients may behave differently in the organism if they are consumed isolately than in conjunction with others. This fact has changed the whole direction of nutritional research. Whereas investigators in the past studied the effect of isolated nutrients (vitamins, minerals, etc.), today the trend is to study whole foods. This approach is much more realistic but also more difficult. This may explain some of the apparent contradictions in the results of different studies. Good examples of this are the “French paradox” related to alcohol, mentioned in the chapter of longevity, and now the “calcium paradox” in relation to osteoporosis. Here is what the WHO says about:
“The paradox (that hip fracture rates are higher in developed countries where calcium intake is higher than in developing countries where calcium intake is lower) clearly calls for an explanation. To date, the accumulated data indicate that the adverse effect of protein, in particular animal (but not vegetable) protein, might outweigh the positive effect of calcium intake on calcium balance.” (Diet, Nutrition, and the Prevention of Chronic Diseases, WHO, 2003, p. 131)
Iron
Many are afraid that a total vegetarian diet (vegan) does not contain sufficient iron. However, the experts of the WHO affirm: “The iron obtained from vegetarian diets may be all in the inorganic form,… However, the absorption of inorganic iron is enhanced by the simultaneous consumption of vitamin C, which is abundant in most plant foods.” (Diet, Nutrition, and the Prevention of Chronic Diseases, WHO, 1990, p. 100)
Vitamin B12
Vitamin B12 or cyanocobalamin is the most chemically complex of all the vitamins. It is important for the normal functioning of the brain and nervous system and for the formation of blood. Vitamin B12 is produced by bacteria; it is not available in plants, except as contamination. “Fermented soy products, such as miso and tempeh, shiitake (dried mushrooms) and algae such as spirulina and nori practically contain no vitamin B12. While these foods are sold in health food stores as excellent sources of B12 and are widely used by the macrobiotic community, they actually contain little, if any B12. Instead they contain analogs of B12 that are not active and may actually block the absorption of true vitamin B12.” (W. Craig, Nutrition and Wellness, p. 218)
For absorption, vitamin B12 must first be combined with the intrinsic factor, a protein made by the parietal cells in the stomach. Then it is absorbed in the small bowel. The large bowel of humans also has bacteria that manufacture vitamin B12 but the place of absorption is already passed. Patients with atrophy of the gastric mucosa or total stomach resection require intramuscular injections.
The requirement of vitamin B12 is very small, less than 1 microgram (μg) daily. The recommendation is 2 μg/day. Since there isn’t a reliable and adequate source of B12 in plant foods, vegans should obtain their dietary needs either from foods fortified with B12 or from the regular use of a vitamin B12 supplement. This is especially important for pregnant or nursing women. Interestingly, not all vegans have a B12 deficiency. Total vegetarians should have their vitamin B12 blood level analyzed.
The Protein Myth
Many are afraid that a total vegetarian diet (vegan) does not contain sufficient protein. However, the experts of the WHO affirm that: “Protein requirements are readily met in children and adults eating a varied diet based predominantly on cereals and pulses, […] There are no known advantages from increasing the proportion of energy derived from protein, and high intakes may have harmful effects in promoting excessive losses of body calcium and perhaps in accelerating an age related decline in renal function.” (Diet, Nutrition, and the Prevention of Chronic Diseases, WHO, 1990, p. 90)
“Although most vegetarian diets meet or exceed the Recommended Dietary Allowances for protein, they often provide less protein than non-vegetarian diets. This lower protein intake may be associated with better calcium retention in vegetarians and improved kidney function in individuals with prior kidney damage. Further, lower protein intakes may result in a lower fat intake with its inherent advantages, because foods high in protein are frequently high in fat also.” (Journal of American Dietetic Association, 1993; 93:1317-1319)
In other words, we could say that the vegetarian diet is not deficient in protein; it is the omnivorous diet that has excess of protein. But what about the quality of plant protein? We learned in the school that animal protein is of high quality and that vegetable proteins do not have all aminoacids. Different plants have different proteins. This is why a vegetarian should have variety in the diet. “Progressively it is recognized that, even in totally vegetarian diets containing a diversity of foods, plant sources tend to complement one another in amino acid supply.” (Diet, Nutrition, and the Prevention of Chronic Diseases, WHO, 1990, p. 19)
“Plant sources of protein alone can provide adequate amounts of the essential and nonessential amino acids, assuming that dietary protein sources from plants are reasonably varied and that caloric intake is sufficient to meet energy needs. Whole grains, legumes, vegetables, seeds, and nuts all contain essential and nonessential amino acids. Conscious combining of these foods within a given meal, as the complementary protein dictum suggests, is unnecessary.” (Journal of American Dietetic Association, 1993; 93:1317-1319)
Here again we see the wisdom of the inspired counsel long before nutrition science existed. E.G. White wrote in 1868: “There should not be many kinds at any one meal, but all meals should not be composed of the same kinds of food without variation.” (Counsels on Diet and Foods, p. 200)
The WHO expert group’s recommendations for a healthy diet are intended for all ethnical groups, rich and poor alike. After considering all circumstances and scientific facts, they came to the following conclusion: “The nutrient goals indicate that the health needs of the population are best met by a high-carbohydrate, low-fat diet, rich in starchy foods (e.g., cereals, tubers, and pulses) and including a substantial intake of vegetables and fruit.” (Diet, Nutrition, and the Prevention of Chronic Diseases, WHO, 1990, p. 158)
We realize that a whole plant based diet is the only one that provides proteins in right amount and proportions, low percentage of fats, but of best quality and free from cholesterol and trans-fatty acids, plenty of complex carbohydrates with fiber and phytochemicals, vitamins and minerals.
We could say that the World Health Organization finally discovered the original diet that God gave to mankind several thousand years ago. “Then God said, ‘I give you every seed bearing plant on the face of the whole earth and every tree that has fruit with seed in it. They will be yours for food.’” (Genesis 1:29)
“Again and again I have been shown that God is trying to lead us back, step by step, to His original design, – that man should subsist upon the natural products of the earth.
Vegetables, fruits, and grains should compose our diet. Not an ounce of flesh meat should enter our stomachs. We are to return to God’s original purpose in the creation of man.” (Counsels on Diet and Foods, p. 380)
“As our first parents lost Eden through the indulgence of appetite, our only hope of regaining Eden is through the firm denial of appetite and passion. Abstemiousness in diet, and control of all the passions, will preserve the intellect and give mental and moral vigor, enabling men to bring all their propensities under the control of the higher powers, and to discern between right and wrong, the sacred and the common.” (Counsels on Diet and Foods, p. 59)

Additional reading: Ministry of Healing, chapter 23 “Diet and Health”.
-o-O-o-
References
| ↑1 | Food and Agriculture Organization of the United Nations. |
|---|
